WHAT WILL THE IMPACT OF NATIONAL HEALTH INSURANCE IMPLEMENTATION BE ON THE ORGANISATIONAL DESIGNS OF HEALTHCARE COMPANIES IN SOUTH AFRICA BOTH PRIVATE AND PUBLIC ORGTOLOGY PERSPECTIVES
By: Dr Timmy Kedijang
INTRODUCTION
Navigating the Shift: NHI’s Impact on South African Healthcare Company Structures and Investment Outlook
The implementation of National Health Insurance (NHI) in South Africa signifies a monumental attempt to reform the nation’s deeply fragmented and inequitable healthcare system. Propelled by a constitutional mandate for universal healthcare access, the NHI Act, signed into law in May 2024, aims to establish a single-payer system, pooling funds to purchase services for all eligible residents, free at the point of care. This report analyses the profound impact of NHI on the organisational designs of both public and private healthcare companies, considering the complex socio-political-economic factors at play.
For the public sector, NHI necessitates significant restructuring, including the establishment of a dominant NHI Fund, new governance bodies, and centralised procurement. Public hospitals and clinics face mandatory accreditation, demanding upgrades in quality, infrastructure, and management, alongside the development of Contracting Units for Primary Healthcare (CUPS). Resource allocation, supply chain management, and human resource models will undergo substantial changes, with an anticipated increased demand for staff, particularly at the primary care level, amidst existing shortages and the threat of professional emigration.
The private sector confronts an existential transformation. Private hospitals will need to contract with the NHI Fund, potentially increasing patient volumes but under regulated fee structures. Medical aid schemes face a drastically reduced role, limited to complementary cover once NHI is fully operational, forcing strategic re-evaluation, consolidation, or diversification. Practitioner networks and individual providers will also need to adapt to new contracting and remuneration models. Integration of IT systems across both sectors will be critical.
The NHI’s journey is fraught with challenges: an unresolved and contentious funding model against a backdrop of fiscal constraints and low economic growth; significant legal challenges questioning its constitutionality and practicality; and deep-seated stakeholder resistance. Early implementation experiences are limited, with CUPS pilot sites being the most notable current initiative. Major healthcare companies are adopting varied strategies, from advocating for alternatives and legal action to focusing on interim affordable offerings and non-acute business growth.
The market predicts a protracted and uncertain transition. Consumer behaviour is marked by anxiety and rising medical aid premiums, while investor sentiment remains cautious, awaiting clarity on NHI’s operational details. The success of NHI hinges on overcoming substantial financial, operational, legal, and political hurdles.
For healthcare organisations, strategic agility, innovation, and a capacity for collaboration will be paramount in navigating this transformative period. The investment outlook remains guarded, with opportunities likely confined to niche areas until greater policy certainty and evidence of sustainable implementation emerge.
HYPOTHESIS 2 X APPLICATION ON THE NHI IMPLEMENTATION
There is no doubt that the implementation of the envisaged National Healthcare Insurance system will introduce protracted uncertainty, complexity, complex consumer behaviour and instability in the healthcare market. The healthcare service providers both private and public will potentially be collapsed into one system which will bring its own confusional state, and market disruptions. The organisations are most likely to find themselves making irrational and unsustainable decisions.
The adoption of Hypothesis 2 X which implements the principle of duality where Perceptive and Projective approaches will have to be adopted on an ongoing basis. The perceptive approach will address the operations which we call process construct whilst the projective approach will address the Strategy which we will refer to project construct.
To survive, the organisations (Public and Private) will have to do only 2 things:
- Activities in relation to healthcare delivery by implementing perceptive, repetitive processes (Operations) and projective, unpredictable project construct (Strategy). From the Orgtology perspective the organisations will be able to perform whilst staying relevant during the uncertain transitional implementation process of NHI.
- They have to provide resources which include people, assets and money.
This article will unpack and clarify the details how the Hypothesis 2 X apply to this important topic of National interest from the South African perspective.
THE NATIONAL HEALTH INSURANCE (NHI) IMPERATIVE IN SOUTH AFRICA
The evidence and analysis will use to address the impact on South African Healthcare company structures and Investment outlook will apply the following methodology to articulate the impact:
Level Zero Model (Hendrikz: 2016) as depicted on figure 1 below
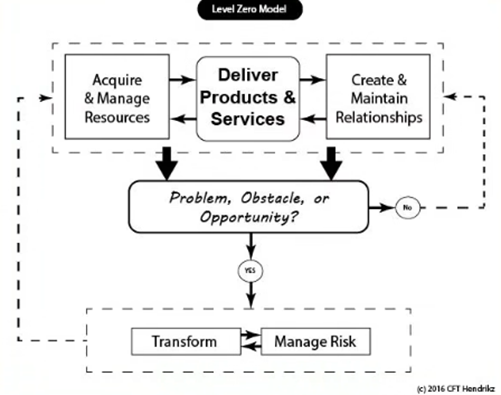
REET Analysis vs Conventional outdated SWOT Analysis:
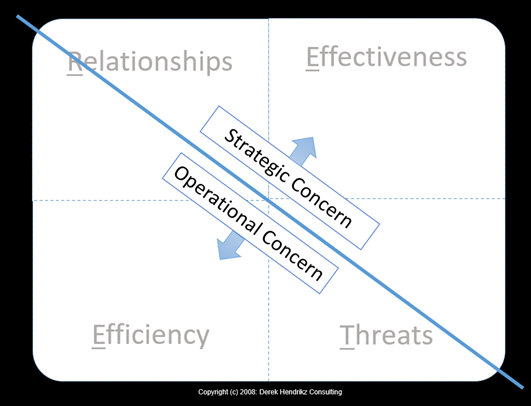
The REET (Relationships, Effectiveness, Efficiency and Threats) as developed by Derek Hendrikz – the founder of Orgtology. It replaces the old conventional SWOT Analysis (Strengths, Weakness, Opportunities and Threats)analysis in phase 2 is a newer adequate way to analyse the reality of an Organisation and should cover both operational and strategic environments to ensure performance and relevance:
There are several assumptions that we can make to relate management and leadership to REET:
- Relationships are needed for both performance and relevance therefore it should be Managed and Led.
- Effectiveness is what Leaders do to work on issue of relevance and strategy.
- Efficiency is what managers work on issue of performance and operations.
- Threats affect both performance and relevance thus they should be both managed and led.
See Figures 2 and 3 below (Hendrikz: 2008)
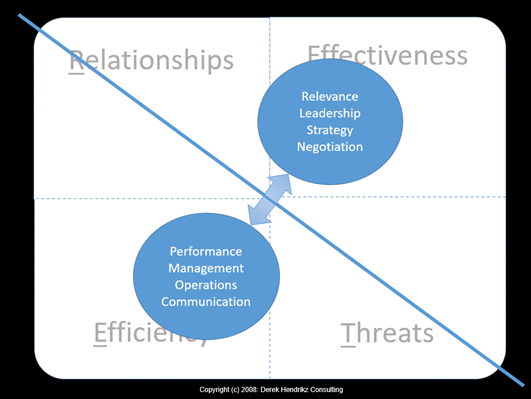
Apply 5V Model
The best way to manage strategy within the organisation is to make sure that vision statements are within reach and not too vague to drive a meaningful strategy. International Orgtology Institute created a simple easy to follow to help organisations to create a ladder of Strategic Success: The 5V Model-creating vision that drives strategy Hendrikz D (2019).
See Fig 4 below illustrating: The 5V Model (Hendrikz: 2008) – An Orgtology Tool
| STATEMENT | TIME SPAN | RECOMMENDED |
| V1 | Ultimate Vision | Our ultimate dream |
| V2 | Long-term Vision | 9 years from now |
| V3 | Medium-term Vision | 6 years from now |
| V4 | Short-term Vision | 3 years from now |
| V5 | Immediate Vision | 12 months from now |
Strategic thinking for the organisation is its ability to anticipate the future, and it always begins with the end in mind. The organisation must use its Orgitelligence (Human and Systems) to take advantage of the changing environment that organisations are operating in. This will ensure Sustainability and Profitability and in Orgtology we call Organizational Intelligence the X- factor which comprised of both Human and Systems Intelligence and must be used to complement.
The National Health Insurance (NHI) imperative in South Africa
Genesis and Rationale: Addressing Systemic Healthcare Disparities South Africa’s healthcare system has long been characterised by a stark “two-tier” structure,
- Market Trends, Behaviour, and Predictions
CONCLUSION: NAVIGATING A PROTRACTED TRANSFORMATION
It is crucial to recognise that NHI’s implementation will be incremental, not an overnight revolution. The journey is fraught with significant hurdles:
-
Financial Unsustainability
The lack of a clear, broadly accepted, and demonstrably affordable funding model in a fiscally constrained economy remains the Achilles’ heel of the NHI. Estimates of its full cost vary wildly, from the government’s R200 billion annually to private sector projections exceeding R1.3 trillion if current private sector care quality were to be universally replicated.
-
Operational Complexity
Reforming entrenched systems, upgrading widespread infrastructure, addressing human resource shortages, and establishing new, efficient administrative bodies are monumental operational tasks.
-
Legal Challenges
Multiple robust legal challenges questioning the NHI Act’s constitutionality and practicality create significant uncertainty and could lead to substantial delays or force major amendments.
-
Political and Stakeholder Dynamics
The post-2024 election political landscape and the need for broader stakeholder buy-in, particularly from healthcare professionals and the private sector, will heavily influence the NHI’s trajectory.
Key uncertainties persist regarding the definitive benefits package to be offered by NHI, the final mechanisms for its funding, and the precise long-term role of medical schemes. These ambiguities will continue to dictate the pace and nature of organisational adaptation.
For public sector entities, the core challenge lies in substantial capacity building, meaningful governance reform to enhance efficiency and accountability, and achieving the required NHI accreditation standards within a tight fiscal environment. Success will depend on strong leadership, effective management, and the ability to overcome historical systemic weaknesses.
For private sector entities, the imperative is strategic agility and innovation. This involves defining their prospective roles within or alongside the NHI framework, developing new service delivery models and product offerings (particularly in the complementary space or for the “missing middle”), rigorously managing financial risks associated with NHI contracting, and potentially exploring diversification.
The broader socio-political-economic climate of South Africa – characterised by high inequality, unemployment, and slow growth – will continue to exert considerable pressure on the NHI’s implementation. Meaningful and sustained collaboration between the public and private sectors, rather than an adversarial approach,
List of Cited Research Material
- Evaluating the potential impact of National Health Insurance on medical scheme members’ rights to have access to health-care services in South Africa, https://scielo.org.za/scielo.php?script=sci_arttext&pid=S2077-49072023000100014
- FAnews, https://www.fanews.co.za/article/healthcare/6/general/1124/government-s-nhi-fix-won-t-work/41274
- Government’s NHI fix won’t work -National Health Insurance (NHI) https://www.health.gov.za/wp-content/uploads/2020/11/some-key-messages-on-nhi.pdf
- Hendrikz D, 2006, http://orgtology.org; Institute of Orgtology
- Hendrikz D, 2008, http://orgtology.org; Institute of Orgtology
- Hendrikz D, 2016, http://orgtology.org; Institute of Orgtology
- Hendrikz D, 2018, http://orgtology.org; Institute of Orgtology
- Hendrikz D, 2020, http://orgtology.org; Institute of Orgtology
- NHI Home National Department of Health https://www.health.gov.za/nhi/
- NHI will bridge gaps in healthcare system and cut costs | South African Government https://www.gov.za/blog/nhi-will-bridge-gaps-healthcare-system-and-cut-cost
- South Africa’s Health Insurance Bill Update | Tennant – Asinta, https://www.asinta.com/news/south-africas-health-insurance-bill-update/
- SOCIO-ECONOMIC IMPACT ASSESSMENT SYSTEM (SEIAS) INITIAL IMPACT ASSESSMENT: National Health Insurance Fund JULY 2017 – Parliamentary Monitoring Group https://pmg.org.za/files/1/NHI_Bill_Socio-Economic_Impact_Assessment_Study.pdf
- Understanding National Health Insurance https://www.hst.org.za/publications/NonHST%20Publications/Booklet%20-%20Understanding%20National%20Health%20Insurance.pdf
- Understanding the National Health Insurance Bill – Securitas https://securitasfinancialgroup.co.za/2024/05/20/understanding-the-national-health-insurance-bill/
- Understanding the National Health Insurance plan – Medirite, https://www.medirite.co.za/health-advice/understanding-the-national-health-insurance-plan.html
- www.health.gov.za https://www.health.gov.za/wp-content/uploads/2023/10/NHI-Frequently-asked-questions-ALL.pdf
By: Dr Timmy Kedijang


